Equipment
Optical Coherence Tomography (OCT)
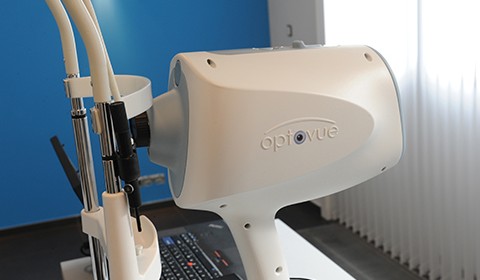
Optical Coherence Tomography (OCT) allows a detailed examination of the macula (macular degeneration, diabetes, venous thrombosis), the optic nerve (glaucoma), and any other specific aspects of the retina. It also allows the examination of the cornea and the irido-corneal angle.
Visual field examination
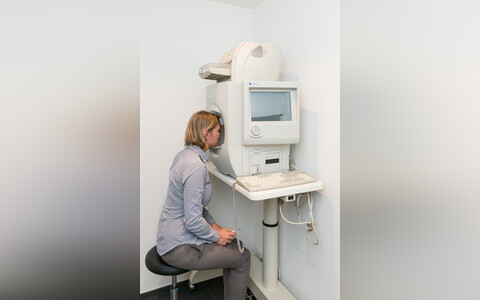
The visual field examination assesses peripheral and central vision by the localization of light dots while fixating a central point. It is used for the assessment of glaucoma, pharmacological toxicity, in case of unexplained visual loss, and to determine fitness to drive.
Optical biometry

The biometric assessment determines the strength of the implant to use to replace the crystalline lens during cataract surgery. Non-contact optical biometry allows the calculation of all types of implants: conventional, toric, multifocal or in case of a previous laser refractive surgery.
Specular microscopy
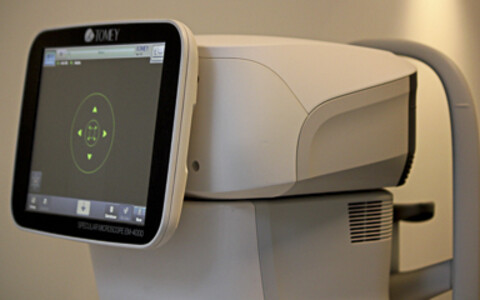
Specular microscopy studies the density and morphology of the corneal endothelium cells.
Topographic keratometry

Topographic keratometry maps the relief and curvature of the cornea. It is used in laser refractive surgery and to detect keratoconus.
Fundus photographs
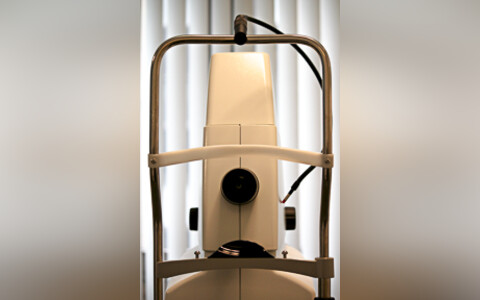
Retinography allows to examine the back of the eye by photos, through filters or dyes (angiography).
Argon Laser

The Argon Laser is used to treat retinopathies (diabetes, venous thrombosis), retinal tears, and certain types of glaucoma.
YAG Laser
The YAG Laser is used for the prevention and treatment of glaucoma as well as for the treatment of secondary cataract.
SLT Laser
The SLT Laser is used for the treatment of some types of glaucoma. It can be used instead of, or in addition to eye drops.
Lancaster test
The Lancaster test is issued to diagnose, assess and follow extra-ocular muscles disturbances.
Retinomax
The Retinomax is used to diagnose and assess eye abnormalities (short-sightedness, far-sightedness, astigmatism) in young children.
